suboccipital muscles and a bad posture
The Epidemic of Forward Head Posture
Forward head posture (FHP) means your head has shifted forward relative to the vertical line of your spine. It has become incredibly common: prolonged screen use and sedentary habits reliably increase its prevalence, and it now affects even children — in 13–15 year-olds, FHP has been found in up to 53.5% of those studied (Tao et al., 2025). Every centimetre your head moves forward adds roughly 4–5 kg of effective load on your neck muscles — a 5 kg head can feel like 15–20 kg to the muscles holding it up.
Four pairs of suboccipital muscles sit in the deepest layer of the neck, right between the base of the skull and the first two vertebrae. They contain an unusually high density of muscle spindles — about 36 spindles per gram of tissue. For comparison, the gluteus maximus has fewer than 1 spindle per gram. This density is not a coincidence: these muscles function less as movers and more as sensors — they continuously tell the brain exactly where the head is positioned (Sung et al., 2022).
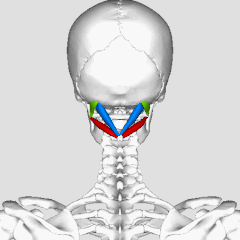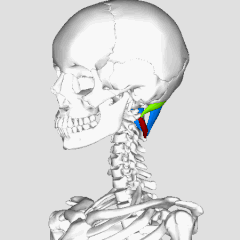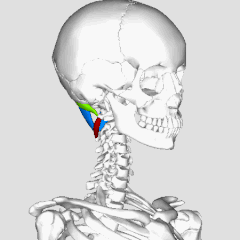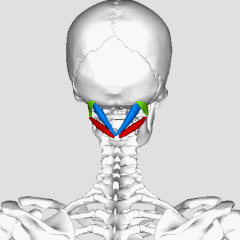
**Try this yourself:** place your fingertips at the base of your skull — right in the hollow between the back of your head and the first vertebrae — and slowly move your eyes from side to side without turning your head. You will feel these tiny muscles gently contracting with every eye movement. This is not a coincidence: the suboccipital muscles are neurally linked to the eye muscles and help coordinate where your gaze points with where your head is turned (the cervico-ocular reflex) (Tarnutzer et al., 2023).
When the Gyroscope Goes Wrong
When these muscles become chronically over-tight — which happens reliably with FHP — their signals no longer match what your inner ear and eyes are reporting. Your brain receives three conflicting streams of information at once. The result is not just neck pain and poor posture, but also dizziness, headaches, and loss of balance (Sung et al., 2022). Research confirms that it is this faulty proprioceptive signal from the neck — not an inner ear problem — that is the primary mechanism behind cervicogenic dizziness, meaning dizziness whose root cause is in the neck, not the ear (Yikilmaz & Buyukturan, 2023).
How Manual Therapy Works
An osteopath or manual therapist works with the suboccipital muscles directly using a technique called suboccipital release. The practitioner slides their fingers under the patient’s skull and holds gentle, steady contact with the suboccipital muscles for 3–5 minutes — no sudden movements. Under sustained pressure the muscles gradually let go. This is myofascial release: excessive tone drops, mobility at the joint between the skull and the first vertebra is restored, and the proprioceptive signal begins to normalise (StatPearls, 2023). A randomised study found that adding suboccipital release to neck flexion exercises produced significantly better improvement in FHP than exercises alone (Doğan et al., 2016).
Another widely used approach is joint mobilisation of the upper cervical spine (such as Mulligan’s SNAGs and passive mobilisation techniques). In a randomised trial with 12-month follow-up, both techniques significantly reduced the frequency and intensity of cervicogenic dizziness, improved neck range of motion, and improved balance — and the effects held up a full year after the treatment course ended (Reid et al., 2014). A 2025 systematic review confirms that manual therapy of the upper cervical spine combined with sensorimotor training — such as head repositioning accuracy drills and eye movement exercises — produces better outcomes than either approach on its own (Rambhia et al., 2025).
How Yoga Works
Yoga complements manual therapy through a different mechanism — gradually re-calibrating the proprioceptive sensors from the inside. Slow, held poses with deliberate attention to sensations in the neck, shoulders, and base of the skull give the muscle spindles and Golgi tendon organs time to rewrite their habitual signal. In a randomised controlled trial, a 12-week yoga programme for patients with chronic neck pain significantly improved the accuracy of head repositioning (a direct measure of proprioception) and reduced trigger point sensitivity — meaning it re-calibrated exactly the sensors that had been sending faulty signals (Cramer et al., 2013).

Lasting postural change is not about “holding yourself straight.” It is about **restoring balanced, optimal muscle tone** and locking in a new movement pattern through regular practice. In a study of people with hyperkyphosis, a 6-month yoga programme produced measurable improvement in scapular position both at rest and during movement — meaning it changed not just how people felt, but the actual mechanics of how they held their body (Cheung et al., 2016).
Why the Combination Works Best
Manual therapy solves the immediate problem: it releases excessive tone, frees up the joint, and gives the nervous system a chance to start receiving accurate signals again. But without regular reinforcement of the new pattern, muscles drift back to their old state — the body remembers what it is used to. Yoga solves the long-term problem: through conscious, slow, and regular movement it updates the motor programmes of the central nervous system, so that the new head position becomes the automatic “normal” — not a constant effort.
Sources
– Tao H et al. 2025. Predictive model for forward head posture in primary school children. _PMC_ 12162659. [https://pmc.ncbi.nlm.nih.gov/articles/PMC12162659/](https://pmc.ncbi.nlm.nih.gov/articles/PMC12162659/)
– Sung YH et al. 2022. Suboccipital muscles, forward head posture, and cervicogenic dizziness. _J Clin Med_ 11(24):7383. [https://pmc.ncbi.nlm.nih.gov/articles/PMC9786116/](https://pmc.ncbi.nlm.nih.gov/articles/PMC9786116/)
– Tarnutzer AA et al. 2023. Cervico-ocular and vestibulo-ocular reflexes in subclinical neck pain. _PMC_ 10670025. [https://pmc.ncbi.nlm.nih.gov/articles/PMC10670025/](https://pmc.ncbi.nlm.nih.gov/articles/PMC10670025/)
– Yikilmaz T, Buyukturan O 2023. Cervical proprioception and vestibular functions in patients with neck pain and cervicogenic headache. _J Turkish Spinal Surgery._ [https://jtss.org/articles/cervical-proprioception-and-vestibular-functions-in-patients-with-neck-pain-and-cervicogenic-headache-a-comparative-study/](https://jtss.org/articles/cervical-proprioception-and-vestibular-functions-in-patients-with-neck-pain-and-cervicogenic-headache-a-comparative-study/)
– StatPearls 2023. Osteopathic Manipulative Treatment: Suboccipital Release. [https://www.ncbi.nlm.nih.gov/books/NBK582126/](https://www.ncbi.nlm.nih.gov/books/NBK582126/)
– Doğan SK et al. 2016. Effects of suboccipital release with craniocervical flexion exercise. [https://pubmed.ncbi.nlm.nih.gov/27261928/](https://pubmed.ncbi.nlm.nih.gov/27261928/)
– Reid SA et al. 2014. Manual therapy for cervicogenic dizziness: long-term outcomes of a randomised trial. _Manual Therapy._ [https://www.sciencedirect.com/science/article/abs/pii/S1356689X14001489](https://www.sciencedirect.com/science/article/abs/pii/S1356689X14001489)
– Rambhia M et al. 2025. Is manual therapy effective for cervical dizziness? Systematic review. _PMC_ 12229031. [https://pmc.ncbi.nlm.nih.gov/articles/PMC12229031/](https://pmc.ncbi.nlm.nih.gov/articles/PMC12229031/)
– Cramer H et al. 2013. Randomized controlled trial comparing yoga and home-based exercise for chronic neck pain. _Clin J Pain._ [https://pubmed.ncbi.nlm.nih.gov/23249655/](https://pubmed.ncbi.nlm.nih.gov/23249655/)
– Cheung C et al. 2016. Yoga Improves Upper-Extremity Function and Scapular Positioning in Persons with Elevated Thoracic Kyphosis. [https://pmc.ncbi.nlm.nih.gov/articles/PMC3965199/](https://pmc.ncbi.nlm.nih.gov/articles/PMC3965199/)
